Abstract
Background: Cervical cancer incidence in Uganda is 54.8 per 100 000 population. We annually treat over 800 new cervical cancers (40% of the workload), which is challenging to treat such numbers in limited resources settings. From July 2011, we commenced the use of hypo-fractionated radiotherapy (HFRT) of 45 Gy/15 fraction (#) as an alternative to conventional fractionated radiotherapy (CFRT) of 50 Gy/25#, for treatment of locally advanced cervical cancer (LACC).
Aim: To compare the 5-year follow-up treatment outcomes between CFRT and HFRT.
Settings: The study analysed patients treated at the Uganda Cancer Institute – a limited resource institution.
Methods: This was a non-randomised, retrospective study, where 414 patients’ files were reviewed according to demographic, clinical, radiotherapy fractionations and outcomes. Inclusion criteria were International Federation of Gynecology and Obstetrics stages IIB–IIIB cervical cancer cases and had completed external beam radiotherapy and intracavitary radiotherapy.
Results: Squamous cell carcinomas were 93.6% and adenocarcinomas were 3.0%. The median age was 49.5 (interquartile range [IQR]: 40.0–56.0) years. Stages IIB/IIIA/IIIB were 36.2%, 8.2%, 55.6%, respectively. Human immunodeficiency virus serology was positive, negative, and unknown in 70 (16.9%), 116 (28.0%) and 228 (55.1%), respectively. Concurrent chemo-radiation was administered in 182 (44.0%) patients. Conventional fractionated radiotherapy and HFRT were 221 (53.4%) and 193 (46.6%), respectively. At 6 months, the overall response rate was 73.3% for CFRT compared with 67.6% for HFRT (p = 0.085), whilst the grades 0–1 toxicities were 94.5% and for 94.7% CFRT and HFRT, respectively (p = 0.080). At 60 months, the survival probabilities were 44.9% for CFRT and 46.6% for HFRT (p = 0.293).
Conclusion: There is no significant statistical difference between CFRT and HFRT for the treatment of LACC. The HFRT could be considered for high volume limited resource settings.
Keywords: cervical cancer; conventional-radiotherapy; hypo-fractionated radiotherapy; limited-resource countries; 5-year survival rate.
Introduction
Cervical cancer is the fourth most common cancer in women worldwide, and the second commonest in developing countries.1 There were 570 000 cases and 311 000 deaths because of cervical cancer in 2018 globally.1 The mortality is 10 times higher in developing countries, where about 80% of new cases occur.2 In the United States (US), most cancer-treatment facilities treat less than three intact cervical cancer patients per year.3 The cervical cancer incidence in Uganda is 54.8 per 100 000 population.1 The Department of Radiotherapy, Uganda Cancer Institute annually treats over 800 new cervical cancer patients, accounting for nearly 40% of the workload; it is challenging to optimally treat such large numbers in centres with limited resources. Locally advanced cervical cancers (LACCs) account for nearly 60% of all cervical patients. Concomitant chemo-radiation therapy is the mainstay of treatment for patients with locally advanced or recurrent cervical cancer.4,5,6 About 65% of patients with stage IIB and 30% – 45% with stage IIIB can potentially be cured.4,7,8
The concept of biologically effective dose (BED) is a measure of true biologically dose delivered by a particular combination of dose per fraction and total dose to a particular tissue. Biologically effective dose is used in radiotherapy to compare and quantify treatment expectations for tumours and normal tissues. The BED is related to the equivalent total doses of 2-Gray (Gy) fractions by the EQD2. The BED normalised in 2.0 Gy fractions, in given by:
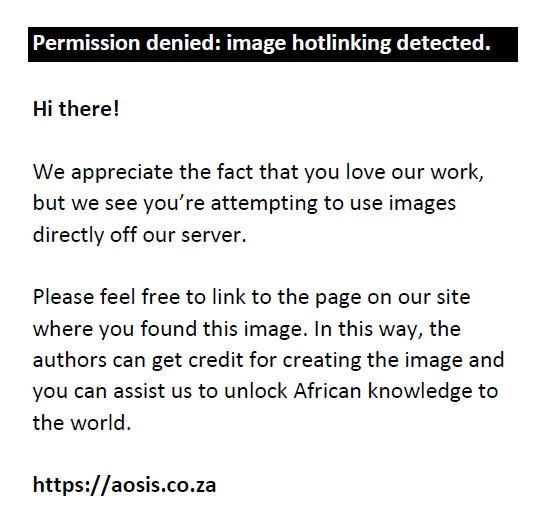
where n is the number of fractions, d is the daily dose, and is the therapeutic ratio.
Assuming an α/β of 10 for early radiation effects (acute toxicity) and tumour response,9,10 50 Gy/25 fraction (#) and 45 Gy/15# have EQD2 values of 50.0 and 48.8, respectively. Assuming an α/β of 3, for the late radiation effects (late toxicity) and organs at risk, 50 Gy/25# and 45 Gy/15# have EQD2 values of 50.0 and 54.0, respectively. For the late radiation effects, assuming an α/β of 3, 50.0 Gy/25# and 45.0 Gy/15# have BED values of 70–84 and 72–90, respectively.
Shuhasis et al.,11 reported on a comparative study that evaluated the role of hypo-fractionated radiotherapy (HFRT) (45.0 Gy/18#) with concurrent weekly Cisplatin versus conventional radiotherapy (50.0 Gy/25#) with concurrent weekly Cisplatin in advanced cervical cancer. No significant difference in response with respect to local regional control and toxicity in both arms was seen. Other than the lower hypo-fractionated dose, the sample size used in this study was very low. Because of the limited treatment facilities and the proximity of the corresponding EQD2 values for tumour response/organs at risk and early/late effects, the department used HFRT of 45.0 Gy/15# as an alternative to the conventional fractionated radiotherapy (CFRT) of 50 Gy/25# from 2011 to 2015. The purpose of this study is to compare the clinical outcomes in patients with locally advanced cervical cancer (stages IIB-IIIB) treated with two regimens of CFRT of 50.0 Gy/25# in 5 weeks and HFRT of 45.0 Gy/15# in 3 weeks. The primary end-points were local control and overall survival.
The referral system is that clinical officers and midwives in health centres II/III are trained to recognise the clinical features of cervical cancer and then refer the patient to health centre IV, where a pap smear/biopsy can be performed. Cancer staging and treatments are carried out at regional and national referral hospitals. At the Uganda Cancer Institute, cervical cancer is managed in the setting of a multidisciplinary team including radiologists, gynaecological-oncologists, medical oncologists, radiation-oncologists, medical physicists, radiation-therapists, oncology nurses, palliative care specialists, etc. involved in management of cervical cancer. The treatment protocol followed the national guidelines for the management and treatment of cervical cancer.12 The cancer treatment is subsidised by the Government of Uganda, and at the time of the treatment. the patients were contributing about $50.00 for the entire course of chemo-radiation treatment.
Materials and methods
Patients and methods
This was a retrospective cohort study of cervical cancer patients staged according to the International Federation of Gynecology and Obstetrics (FIGO) IIB–IIIB2 who received radiotherapy at the centre from January 2011 to December 2012. All data were collected after approval from the Research and Ethics Committee of the Uganda Cancer Institute. Inclusion criteria were patients with histologically confirmed cervical cancer and had completed both the planned external beam radiotherapy (EBRT) and intra-cavitary (ICT) treatments. A total of 417 LACC patient’s files, FIGO stages IIB-IIIB were reviewed in 2020. The review was according to the demographic and clinical data, treatment waiting time (calculated as the time between the patient’s registered date in department and the date of the first EBRT treatment), treatment fractionations, toxicities, responses and 5-year survival probabilities. In addition to the information retrieved from the files, the researchers also made phone calls to get current patient status/updated information from the patient or next of kin. We developed and tested a REDCAP – for online project data collection tool.
Chemo-radiation
Pre-treatment evaluation and staging included detailed history, thorough clinical examination including bimanual pelvic examination, chest radiograph, trans-abdominal/pelvic ultrasound, digital rectal examination, complete blood count, liver and renal functional tests. A similar protocol was followed during external beam simulation, target delineation, 2D treatment planning, and treatment with patient in supine position.13 Radiation field borders were: (1) superiorly: L4-L5 inter-disc space; (2) inferiorly: below the obturator foramina or 3 cm below the inferior extent of the vaginal disease; and (3) laterally: 1 cm – 2 cm lateral to the true pelvis. About 30 min, before conventional simulation and daily treatments, patients were advised to drink 500 mL of water, to minimise bladder toxicity. The EBRT was delivered by parallel opposed anterior-posterior and posterior-anterior portals using a Cobalt-60 beam. The planned regimen included whole pelvis EBRT, administered as 50 Gy/25# for the CFRT and 45 Gy/15# for the HFRT regimen. All patients referred from January 2011 to June 2012 were treated with the CFRT regimen and those referred from July 2012 onwards were treated with HFRT regimen. Patients with anterior-posterior separation of more than 22.0 cm were treated with the CFRT regimen. Weekly Cisplatin of 40 mg/m2 was administered to patients deemed fit for concurrent chemo-radiation,5,6,13 irrespective of their sero-status. Weekly CBC (Haemoglobin ≥ 10.0 g/dL), Urea and creatinine levels were checked prior to chemo administration. The cut-off CD4 level was 200 cells/mm3 for the human immunodeficiency virus (HIV) seropositives. The EBRT was followed with a single insertion of low-dose-rate Cs-137 ICT delivering 30 Gy to point A. Patients were offered the departmental follow-up protocol; first review at six weeks, then every three months for the first six months, six months up to one year and 12 months thereafter up to 60 months.
Assessment of treatment outcomes
The analysis was according to age at diagnosis, histology, degree of differentiation, Eastern Cooperative Oncology Group (ECOG) status, HIV serology, radiation dose, ± Cisplatin, ICT, tumour response at ICT, treatment duration, response and complications during EBRT/follow-up, retreatments in the 5-year period and survival probabilities. The retreatments were palliative doses, for example, 10.0 Gy/1#, 20.0 Gy/5# or 20 Gy single dose of Cs-137 insertion to point A. The study also evaluated the delays in the clinical workflow of the radiotherapy process, starting from when the patient is registered, doctor-clerking, planning/simulation to the first fraction of treatment delivery. The response to EBRT was assessed basing on the clinical information documented in the patient’s files while on treatment, at the time of ICT, and subsequent follow-up visits. At the time of ICT, the attending doctor documented whether there was no residual (clinically visible) tumour, if there was a presence of tumour – its size and presence of discharge or bleeding. This information was used to score response basing on the RECIST criteria14 as: SD = stable disease, PR = partial response, CR = complete response, DP = disease progression at ICT. The scoring was: CR for no tumour seen, PR for tumour < 1.5 cm diameter, SD for tumour > 1.5 cm, and DP for necrotic/bleeding tumour filling the cervix. The information given by the patient on subsequent visits, for example, no complaint, pain, discharge, bleeding and visual speculum examination were used to score the patient’s case as SD, PR, CR and DP on follow-up. The overall response rate (ORR) was defined as the proportion of patients who had PR or CR to the treatment.
The treatment-related side effects were evaluated using Radiation Therapy Oncology Group (RTOG) criteria,15 based on skin reactions, gastrointestinal and genitourinary complications as documented in the patient’s file. The toxicities were graded as:
- Grade 0: no complications or symptoms
- Grade 1: (mild toxicity), for example, increased urinary/bowel frequency, anorexia, nausea, vomiting, mild abdominal and rectal pains, dry desquamation
- Grade 2: (moderate toxicity) moderate diarrhoea, moderate abdominal and rectal pains, intermittent bleeding
- Grade 3: Skin ulceration, bloody stool and GI bleeding, fibrosis, obstruction
- Grades 4: (severe toxicity), for example, severe abdominal pains, wet desquamation, necrosis and fistula.
Statistical analysis
The sample size was determined using the Leslie Kish formula, which is appropriate for comparison between two groups when endpoint is qualitative and the minimum for each group was 135 patients’ cases. However, this study being retrospective, we preferred the inclusion of all patients in the study period. All statistical analyses were performed using a statistical software package (STATA version 12). Quantitative data were presented by numbers, percentages and median as appropriate. Survival rates were computed using the Kaplan–Meier method. A p-value < 0.05 was considered statistically significant. Other statistical parameters included: p-values and inter-quartile range (IQR).
Ethical considerations
This study is a retrospective review. The project was approved by the Uganda Cancer Institute Research and Ethics Committee (UCIREC reference 05-2020).
The use of patients’ data was approved by the Uganda Cancer Institute Research and Ethics Committee. All methods were performed in accordance with the relevant guidelines and regulations.
Results
Figure 1 shows study’s inclusion and exclusion diagram.
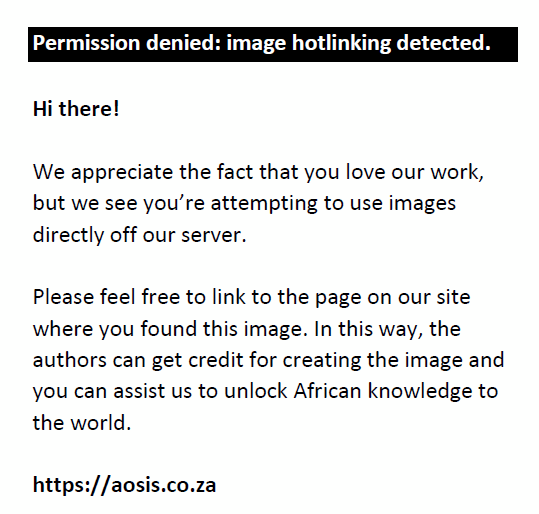 |
FIGURE 1: Inclusion ad exclusion criterion of the patients. |
|
Histological results were squamous cell carcinoma (SCC) poorly, moderately, well differentiated, adenocarcinoma and others, contributing 38.2%, 26.3%, 19.8%, 2.6%, 13.1%, respectively. The age ranged from 24 to 80, with a median of 49.5, and peak age-group of 40–49 years. Stages IIB, IIIA and IIIB were 36.2%, 8.2% and 55.6%, respectively. The HIV serology was positive, negative and unknown in 70 (16.9%), 116 (28.0%) and 228 (55.1%), patients respectively. Of those whose serology statuses were known, 62.4% were negative and 37.6% were positive. Patients ECOG status were categorised as 0, 1 and 2, contributing 1.2%, 85.0% and 13.8%, respectively. The median waiting time to start EBRT was 11.0 (IQR: 4.0–21.0 days). Concurrent chemotherapy was administered in 182 (44.0%) patients and only 93 (51.2%) of these completed the prescribed number of cycles. Logistical reasons (83.8%) were the main cause for not completing the prescribed chemotherapy followed by clinical factors (17.8%). Table 1 shows the demographic, clinical and pathological characteristics of all patients included in the review. The number of patients with anterior–posterior separation ≥ 22.0 cm were 15 (3.6%) – they were all treated with the CFRT regimen. The median treatment duration was 55.0 days (IQR: 40.0–81.0 days) for HFRT compared with 65.0 days (IQR: 52.0–84.0 days) for CFRT. At ICT, 9.1%, 36.0%, 48.6%, 0.8% had SD, PR, CR and DP for CFRT compared with 12.6%, 41.3%, 38.1%, 0.8% for HFRT (p = 0.193). Table 2 shows a summary of response and follow-up at different periods, chosen as per departmental follow-up protocol. At six months, the ORR was 73.3% for CFRT compared with 67.6% for HFRT (p = 0.085). Table 3 summarises the toxicities at different periods. At six months, the grades 0–1 toxicities were 94.5% and for 94.7% CFRT and HFRT, respectively (p = 0.080). Only 38.1% patients in the CFRT completed the total prescribed dose (EBRT + ICT) within the intended treatment time of 7–8 weeks compared with 50.8% in the HFRT who completed intended treatment time within 5–6 weeks. Re-treatments during the 5-years of follow-up were 10.4% and 7.8% for CFRT and HFRT, respectively (p = 0.354). At five years, the survival probabilities were 44.9% for CFRT compared with 46.6% for HFRT (p = 0.293). The study also evaluated the survival probability patterns for patients with known HIV serology (HIV-positive vs. HIV-negative), stage IIB, IIIA, IIIB and patients less than 50 years versus those more than 50 years of age. Figure 2a–d shows their corresponding Kaplan-Meier survival probabilities. The results show that the 5-year survival probabilities for stage IIB, IIIA and IIIB patients were 56.0%, 42.4% and 38.1%, respectively. The corresponding p-values are: IIB versus IIIB = 0.002, IIB versus IIIA = 0.005 and IIIA versus IIIB = 0.415. The 5-year survival probabilities for HIV-positive and HIV-negative were 30.6% and 44.9%, respectively (p = 0.021). The 5-year survival probabilities for patients < 50 years and those ≥ 50 years of age were 37.9% and 51.8%, respectively (p = 0.008). Table 4 shows a comparison stage according to patient’s age at presentation.
| TABLE 1: Clinical and pathological characteristics of all included patients in the review. |
| TABLE 2: Summary of response at intra-cavitary and follow-up at different periods. |
| TABLE 3: Summary of toxicities at different follow-up periods. |
| TABLE 4: Comparison of stage according to patients’ age at presentation. |
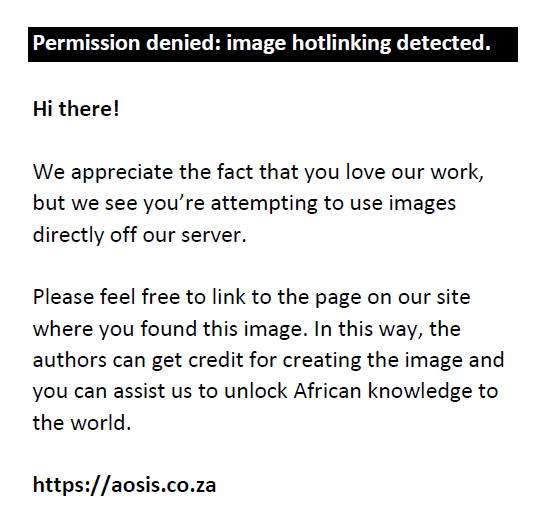 |
FIGURE 2: Kaplan–Meier survival probability comparison for (a) CFRT versus HFRT, (b) HIV negative versus positive, (c) FIGO stage IIB, IIIA, IIIB (d) age < 50 versus ≥ 50 years. |
|
Discussion
The retrospective analysis of CFRT versus HFRT regimens shows that the 5-year overall survival (OS) for CFRT and HFRT were 44.9% and 46.6%, respectively (differences are statistically insignificant (p = 0.293). At 60 months of follow-up, the tumour control rates and survival probabilities were comparable between CFRT and HFRT. There were significant statistical differences in toxicity at 3–6 months of follow-up. but were limited to grades 0 (no complaint) – grade 1 (mild symptoms). The average 5-year survival probability of 45.8% patients in this study is lower than 58.0% published by other studies,7,8 for locally advanced cervical cancer. A number of factors may contribute to this, for example, not completing the prescribed treatments (EBRT, ICT and chemotherapy) within the stipulated times, high prevalence of HIV within the patients, inadequate treatment resources, etc. During treatment, the toxicities were mainly mild for both CFRT and HFRT, whilst during follow-up, the toxicities ranged from no complaint to mild. The grade 3 – 4 treatment-related toxicity profiles for both groups in our study are much lower than other studies16,17 that reported values in range of 18.0% – 21.6%. Our study being retrospective, it is possible that severe toxicities could have been missed. McArdle et al.18 reported that toxicity profiles were lower in sub-Saharan African countries. As shown in Table 3, for the first 3–6 months of follow-up, the proportions of patients with no complaint as expected were higher for CFRT compared with HFRT (p = 0.016). After 1 year of follow-up, the toxicity profiles became comparable. The outcomes in our study may not adversely change, based on a 10-year follow-up retrospective study of 442 cervical cancer patients with stage IIB-IVA after radiotherapy.19 This study showed that early treatment-related side-effects occur within the first 3 months and almost half of the patients developing late recto-sigmoid and bladder complications did so within the first year after treatment, with almost all complications developing within 3–4 years after radiotherapy. This is in agreement with our results shown in Table 2, where the grade 3–4 toxicities were observed within the first 24 months. A retrospective 30-year follow-up of 1456 patients (stages IB-IVA) treated with EBRT and ICT to doses in the range of 70–90 Gy indicated that the incidence of significant morbidity was closely correlated with doses higher than 80 Gy.20 The dose ranges of 75–80 Gy used in our study are subsequently not expected to cause grave side effects.
The results show that SCC was the commonest histology, in agreement with known literature. The mean age at diagnosis of about 50 years agrees with other literature reviewed.8 The HIV sero-status was known in 46.6% patients in CFRT compared with 43.0% in HFRT, and of these 18.1% and 15.5% were positive, respectively. A large portion of patients had no HIV-serology results because at that time, screening was of voluntary testing compared with routine testing practiced currently. In this study, the seropositives are nearly 40% compared with 7.1%, which was the HIV/AIDS prevalence rate for women aged 15 years and above, around that time in Uganda.21 This could be attributed to both HIV and cervical cancer being sexually transmitted, with patients who are infected with HIV having a higher risk of having humanpapilloma virus (HPV) infection as well.
Most of the patients were in ECOG 1–2, other higher ECOG status were not observed in the review as those patients were frail for radical treatments. Concurrent chemo-radiation was administered in 44.0% patients and only 51.2% of these completed the prescribed number of cycles. Logistical reasons (83.8%) were the main cause for not completing the prescribed chemotherapy followed by clinical factors (17.8%). Most patients had stage IIIB disease (52.7%) with hydronephrosis, raised serum creatinine levels and end stage renal failure, where Cisplatin-based chemotherapy is contraindicated. McArdle et al.18 reported that more than 60% of the cervical cancer patients in sub-Saharan Africa were ineligible for chemotherapy at presentation, which is in agreement with our results.
As much as the results in Table 4 show that there is a noticeable presentation of young age group 20–29 with more advanced stage IIIB disease, the overall comparison of patients’ age and stage at presentation is not statistically significant (p = 0.940). Further analysis, however, showed that young (age < 50 years) patients had poor outcomes in terms of response and survival probabilities, compared with older patients (age ≥ 50 years) and the differences are statistically significant (p = 0.008). This agrees with other studies,22,23 which showed that young age was an unfavourable prognostic factor, especially in more advanced stages. On the contrary, Gao et al.24 showed that cervical cancer had the same prognosis in the elderly as well as the young women.
There was a significant survival difference between the HIV seronegative and HIV seropositive patients (44.9% vs. 30.6%, p = 0.021). Gichangi et al.25 reported that HIV infection was significantly associated with higher risk of residual tumour post-EBRT. The serology results can be correlated with patients’ age, as the younger generations are more sexually active, hence more prone to HIV infection. Our results show that the median (IQR) age for HIV seropositive patients was 42.0 (9.0) compared with 49.5 (13.0) for HIV seronegatives. The survival probability for seropositive patients has substantially improved compared with that seen about two decades ago at the centre. In this analysis, the 2-year survival probabilities for seropositive was 61.4% in comparison with a previous study,26 where the 2-year survival probability for seropositive was 40.0%. The improvement can partially be attributed to the increased use of free antiretrovirals (ARVs), which are known to enhance the patient’s general well-being. The immune-status of seropositive patients in this study was much higher, with average cluster of differentiation 4 (CD4)counts of 444 (±246 standard deviation [s.d.]) cells/mm3 compared with the previous study, where it was 289 (±122 s.d.) cells/mm3.
There was a significant survival difference between stage IIB and stages IIIA / IIIB (56.0% vs. 42.4% / 38.1% with p-values of 0.005 / 0.002). The survival probabilities in this study for stage IIB and IIIB are much lower compared with other published data8,27 that showed values of about 75% and 60%, respectively. The treatment outcomes in this analysis could be compromised by the long treatment duration (EBRT + ICT), as it is well known that the overall treatment time should be kept as short as possible (preferably less than 56 days) for conventional fractionation.4 This problem was aggravated by having one low-dose-rate Cs-137 unit, resulting in long waiting times for patients to receive brachytherapy.
The proportion of patients who completed the prescribed radiation dose in the intended time was low in both groups, but much worse in the CFRT group. Factors that majorly contributed to this include: One low-dose-rate (LDR) ICT unit that can treat maximum two patients per day, EBRT machine breakdown and patients’ socio-economic factors. Patient-related logistical issues such as accommodation, transport, feeding, etc. affected some patients not to complete their prescribed treatments on time. The addition of chemotherapy to a hypo-fractionated treatment may have caused negligible toxicity concern, as the HFRT group treatment completion rate was higher compared with the CFRT.
Limitations of this study
- Treatments were 2-fields (anterior-posterior [AP] and posterior-anterior [PA]) 2D treatment planning:
- Conformal 4-field techniques are preferable especially when utilising HFRT.
- Inability to escalate dose to ≥ 80.0 Gy from both EBRT and ICT, which may be required for most of the LACC.
- Treatments were carried out on Cobalt-60 unit with relatively low dose rate (≈0.6 Gy/min) – patient’s movements during the long treatment times may affect response.
- Some patients inappropriately received chemotherapy during radiation therapy treatment (e.g. partially received, during weekends, after radiation course).
- Often the brachytherapy insertions were not received within the stipulated time – the then available low-dose rate Caesium-137 unit could treat at most two patients per day.
- A comprehensive toxicity profiles especially the adverse treatment related side effects could have been unnoticed.
- This has been a retrospective cohort study, mainly observational and descriptive. This allows limited preliminary commentary on the equivalence or non-inferiority of HFRT versus CFRT for the treatment of LACC.
Our department is to start a prospective randomised trial to evaluate a HFRT 45.0 Gy/15# schedule of radiotherapy delivered in 3 weeks versus the CFRT 50.0 Gy/25# regimen delivered in 5 weeks for the treatment of LACC. All patients will be treated with IMRT photon energies 6 mega-voltage (MV) or 10 MV, with weekly chemotherapy (Cisplatin 40 mg/m2 weekly) followed by brachytherapy (HDR 8.0 Gy × 3#) to point A, once a week for three fractions starting in the last week of pelvic EBRT. The objective will be to compare the short-term clinical outcomes in patients with LACC treated with the two regimens. There are currently two National Institutes of Health prospective phase II, randomised clinical trials, comparing concomitant chemotherapy CFRT with HFRT, followed by brachytherapy, enrolling cervical cancer patients.28,29 The first28 compares 50 Gy/25# with 37.5 Gy/15#, plus brachytherapy 28 Gy to point A with weekly Cisplatin. The second29 compares 45.0 Gy/25# with 40.0 Gy/15#, plus brachytherapy with weekly Cisplatin.
The shorter regimen of 45.0 Gy/15# can be beneficial in several ways to both the patients and the institutions providing the healthcare , for example: (1) The overall machine time is shorter with HFRT, therefore resulting into reduced time patients take whilst waiting to start EBRT. (2) HFRT can result in better patient compliance, because of shorter hospital stays. (3) For the hospitals, more patients are treated in the same time period, hence saving on resources.
Conclusion
No significant statistical differences were noticed in tumour response and survival rates in this study of patients with LACC treated with either CFRT or HFRT. There were statistical differences at 3–6 months, limited to grades 0 (no complaint) – grade 1 (mild symptoms). In high volume cervical cancer patients’ and low resource settings, the shorter regimen of 45 Gy/15 fractions can be beneficial to both the patients and the institutions providing the healthcare; hence it should be considered because of its resource friendliness and convenience to the patients. Furthermore, prospective, randomised studies and conformal radiotherapy treatments are needed in the exploration of better management of locally advanced cervical cancer in limited resource settings. There is also a need to investigate if there are biological differences between the tumours seen in the young and the older patients or if it as a result of the HIV ,and whether these need to be addressed differently.
Acknowledgements
- Mr Mulumba Yusuf: A biostatistician for his help in data management and analysis
- Dr. Kanyike Daniel: A consultant radiation oncologist and Head of Radiotherapy Department for his administrative guidance and encouragement
Competing interests
The authors declare that they have no competing interests and have no financial or personal relationship that may have inappropriately influenced them in writing this article.
Authors’ contributions
This research was realised by A.K. and I.L. who were mainly involved in research initiation, data collection, analysis and write-up. C.B. was involved in data collection and analysis. S.K. was involved in data analysis and the final write-up.
Funding information
This work was supported by the Varian Medical Systems Inc., Palo Alto, California, United States.
Data availability
Raw and derived data supporting the findings of this study were generated at the Department of Radiotherapy, Uganda Cancer Institute. The data that support the findings of this study are available on request from the corresponding author, A.K.
Disclaimer
The views and opinions in this article are those of the authors and do not reflect the official position or policy of any affiliated agencies of the authors, and the Publisher.
References
- GLOBOCAN. Estimated cancer incidence, mortality and prevalence worldwide [homepage on the Internet]. [cited 2021 Apr 2]. Available from: www.globocom.iarc.fr 2020
- Haie-Meder C, Morice P, Castiglione M. Cervical cancer: European Society of Medical Oncologist – Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2010;21(5):37–40. https://doi.org/10.1093/annonc/mdq162
- Eifel PJ, Ho A, Khalid N, Erickson B, Owen J. Patterns of radiation therapy practice for patients treated for intact cervical cancer in 2005 to 2007: A quality research in radiation oncology study. Int J Radiat Oncol Biol Phys. 2014;89(2):249–256. https://doi.org/10.1016/j.ijrobp.2013.11.228
- Keys H, Gibbons SK. Optimal management of locally advanced cervical carcinoma. J Natl Cancer Inst Monogr. 1996;21:89–92.
- Chung YL, Jian JJ, Cheng SH, et al. Extended-field radiotherapy and high-dose-rate brachytherapy with concurrent and adjuvant cisplatin-based chemotherapy for locally advanced cervical cancer: A phase I/II study. Gynecol Oncol. 2005;97(1):126–135. https://doi.org/10.1016/j.ygyno.2004.12.039
- Rose PG, Ali S, Watkins E, et al. Long-term follow-up of a randomized trial comparing concurrent single agent cisplatin, cisplatin-based combination chemotherapy or hydroxyurea during pelvic irradiation for locally advanced cervical cancer: A Gynecologic Oncology Group Study. J Clin Oncol. 2007;25(19):2804–2810. https://doi.org/10.1200/JCO.2006.09.4532
- American Cancer Society. Survival Rates for Cervical Cancer [homepage on the Internet]. [cited 2021 Apr 9]. Available from: https://www.cancer.org/cancer/cervical-cancer/detection-diagnosis-staging/survival.html
- Cancer.Net. [cited 2021 Apr]. Available from: https://www.cancer.net/cancer-types/cervical-cancer/statistics
- Perez CA, Brandy LW, Halperin EC, Schmidt-ullrich RK. Principals and practice of radiation oncology. In: Halperin EC, Schmidt-ullrich RK, Perez CA, Brandy LW, editors. Overview and basic science of radiation oncology. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins, 2004; p. 26–32.
- Wang CJ, Huang EY, Sun LM, et al. Clinical comparison of two linear-quadratic model-based isoeffect fractionation schemes of high-dose-rate intracavitary brachytherapy for cervical cancer. Int J Radiat Oncol Biol Phys. 2004;59(1):179–189. https://doi.org/10.1016/j.ijrobp.2003.10.025
- Subhasis M, Niharika P. A Comparative study to evaluate the role of Hypofractionated radiotherapy with concurrent weekly Cisplatin Vs conventional radiotherapy with concurrent weekly Cisplatin in advanced carcinoma Cervix. Sch J App Med Sci. 2017;5(7D):2809–2816.
- Kiguli-Malwadde E, Gakwaya AM, Robinson AJ, Kigula-Mugambe JB, Luwaga AK. Cancer of the cervix: The Uganda Guidelines. East Cent Afr J Surg. 2005;10(2):93–99.
- Gandhi AK, Sharma DN, Rath GK, et al. Early clinical outcomes and toxicity of intensity modulated versus conventional pelvic radiation therapy for locally advanced cervix carcinoma: A prospective randomized study. Int J Radiat Oncol Biol Phys. 2013;87(3):542–548. https://doi.org/10.1016/j.ijrobp.2013.06.2059
- National Cancer Institute (NIH). Response evaluation criteria in solid tumors (RECIST) [homepage on the Internet]. [cited 2021 Apr 16]. Available from: https://www.cancer.gov/publications/dictionaries/cancer-terms/def/recist
- Cox JD, Stetz J, Pajak TF. Toxicity criteria of the Radiation Therapy Oncology Group (RTOG) and the European Organization for Research and Treatment of Cancer (EORTC). Int J Radiat Oncol Biol Phys. 1995;31(5):1341–1346. https://doi.org/10.1016/0360-3016(95)00060-C
- Jakubowicz J, Blecharz P, Skotnicki P, Reinfuss M, Walasek T, Luczynska E. Toxicity of concurrent chemoradiotherapy for locally advanced cervical cancer. Eur J Gynaecol Oncol. 2014;35(4):393–399.
- Tan LT, Zahra M. Long-term survival and late toxicity after chemoradiotherapy for cervical cancer – The Addenbrooke’s experience. Clin Oncol. 2008;20(5):358–364. https://doi.org/10.1016/j.clon.2008.03.001
- McArdle O, Kigula-Mugambe JB. Contra-indications to cisplatin based chemotherapy in the treatment of cervical cancer in Sub-Saharan Africa. Radiother Oncol. 2007;83(1):94–96.
- Perderson D, Bentzen SM, Overgaard J. Early and late radiotherapeutic morbidity in 442 consecutive patients with locally advanced carcinoma of the uterine cervix. Int J Radiat Oncol Biol Phys. 1994;29(5):941–952. https://doi.org/10.1016/0360-3016(94)90387-5
- Perez CA, Grigsby PW, Lockett MA, Chaos KS, Williamson J. Radiation therapy morbidity in carcinoma of the uterine cervix: Dosimetric and clinical correlation. Int J Radiat Oncol Biol Phys. 1999;44(4):855–866.
- United Nations Programme on HIV/AIDS (UNAIDS). Country factsheet: Uganda, HIV and AIDS estimates [homepage on the Internet]. [cited 2021 Apr 23]. Available from: https://www.unaids.org/en/regionscountries/countries/uganda
- Chen RJ, Lin YH, Chen CA, Huang SC, Chow SN, Hsieh CY. Influence of histologic type and age on survival rates for invasive cervical carcinoma in Taiwan. Gynecol Oncol. 1999;73(2):184–190. https://doi.org/10.1006/gyno.1999.5364
- Polterauer S, Grimm C, Hofstetter G, et al. Nomogram prediction for overall survival of patients diagnosed with cervical cancer. Br J Cancer. 2012;107:918–924. https://doi.org/10.1038/bjc.2012.340
- Gao Y, Ma J, Gao F, Song L. The evaluation of older patients with cervical cancer. Clin Interv Aging. 2013;8:783–788. https://doi.org/10.2147/CIA.S45613
- Gichangi P, Bwayo J, Estambale B, et al. HIV impact on acute morbidity and pelvic tumor control following radiotherapy for cervical cancer. Gynecol Oncol. 2006;100(2):405–411. https://doi.org/10.1016/j.ygyno.2005.10.006
- Kigula-Mugambe JB, Kavuma A. Effect of HIV serological status on outcome in patients with cancer of cervix treated with radiotherapy. East Afr Med J. 2006;83(8):416–423. https://doi.org/10.4314/eamj.v83i8.9455
- Texas Oncology. Stage II Cervical Cancer [homepage on the Internet]. [cited 2021 Apr 16]. Available from: https://www.texasoncology.com/types-of-cancer/cervical-cancer/stage-ii-cervical-cancer
- NIH Clinical trials. Chemotherapy and pelvic hypofractionated radiation followed by brachytherapy for cervical cancer [homepage on the Internet]. [cited 2021 Apr 30]. Available from: https://clinicaltrials.gov/ct2/show/NCT04070976
- NIH Clinical trials. Hypofractionated External beam Radiotherapy for Intact Cervical Cancer (HEROICC) [homepage on the Internet]. [cited 2021 Apr 30]. Available from: https://clinicaltrials.gov/ct2/show/NCT04583254
|





