Abstract
Purpose: Treatment options for acoustic neuromas (ANs) are limited in low- and middle-income countries. The aim of this study was to investigate whether hypofractionated image-guided radiotherapy (IGRT) is a clinically acceptable treatment option for departments where no other radiosurgery options are available.
Methods and materials: Fifteen dynamic conformal arc plans that had been clinically utilised were evaluated against the Radiation Therapy Oncology Group (RTOG) radiosurgery criteria and published indices. Analysis involved evaluating critical structure doses and the volume of normal tissue receiving 12 and 10 Gy single fraction equivalent dose (V12Eq and V10Eq).
Results: Overall, there was only one RTOG protocol deviation in the whole patient group, where quality of coverage was compromised in order to achieve brainstem tolerance. Conformity indices were within clinically acceptable limits (CIPaddick ≥ 0.6) despite being inferior to the published Universitair Ziekenhuis Brussel (UZB) Gamma Knife and CyberKnife results (p < 0.0001). Homogeneity was superior to the Gamma Knife (p < 0.0001) and Novalis dynamic conformal arc (p = 0.0002) results. Gradient index results were inferior to all published techniques, but doses to the normal structures were well controlled with the exception of the cochlea. The V10Eq data showed increased sensitivity when compared with V12Eq.
Conclusion: Dynamic arc IGRT allows for good coverage of AN lesions, but the dose fall-off is not as steep as that obtained with mainstream radiosurgery systems. Contouring and planning should include detailed critical structures analysis. For normal brain parenchyma analysis, V10Eq is a superior risk indicator when compared to V12Eq for this technique. Dynamic arc IGRT offers a dosimetrically acceptable treatment alternative for patients without serviceable hearing, in departments where there are no mainstream radiosurgery treatment options available.
Introduction
Acoustic neuromas (ANs) or vestibular schwannomas are benign neoplasms associated with the vestibular cranial nerve. Although benign, untreated lesions may cause symptoms because of local nerve compression of the auditory, vestibular, facial or, less commonly, the trigeminal nerve.1,2 Very large lesions may become life-threatening because of brainstem compression.
Historically, surgery was considered the treatment of choice, but the introduction of stereotactic radiosurgery in the latter half of the 20th century allowed for significantly lower levels of morbidity and similar or better levels of tumour control.3 Radiosurgery is less invasive than surgery and can be performed on outpatients, making it the preferred choice for many. Radiosurgery is commonly used as the favoured treatment option for small to medium ANs.4
Access to radiosurgery in resource-constrained low- and middle-income countries (LMICs) is poor. The equipment required is expensive and often unavailable. It is estimated that there is one Gamma Knife radiosurgery unit in Africa per 370 million people.5 There are no CyberKnife units in Africa.
As an alternative to Gamma Knife and CyberKnife units, linear accelerators (linacs) can be modified to improve delivery accuracy and the ability to focus beams, thus allowing for their use in radiosurgery treatments. The positional accuracy of modified linacs is reported to be within 1 mm.3
There are currently 139 countries classified as LMICs by the World Bank. An analysis revealed that only four LMICs had the required number of linacs for radiotherapy treatment: 55 of the 139 LMICs had no access to radiotherapy treatment at all (40 in Africa), while 80 had some level of access.6 Over 60% of linacs in Africa are situated in South Africa and Egypt.7 Even in South Africa, it is estimated that only 69.7% of the required number of linacs are installed, and that an additional 56 will be required by 2020.6 Very few linacs in South Africa are modified for radiosurgery treatment.
A survey performed at Groote Schuur Hospital (Cape Town, South Africa) in 2013 to determine the level of access to radiosurgery in South Africa found that there were no Gamma Knife or CyberKnife units in the country.8 Proton-based radiosurgery was introduced to the country in 1993, followed by the first linac-based radiosurgery in 1994. More than 2300 patients were treated between 1993 and 2012. Proton-based radiosurgery was used for 22.6% of patients, with 71.4% treated on five modified linacs operating within the private hospital sector. Although 84% of the South African population are treated in state facilities, with no access to private medical facilities, only 6% of the total number of radiosurgery treatments were performed within state sector facilities because of limited resources.8,9
Groote Schuur Hospital (GSH) has offered limited radiosurgery to state patients since 2008, treating 25 between 2008 and 2012 using a second-hand Radionics cone-based radiosurgery system. This broke down and became obsolete in 2012, and a new replacement system was not financially possible. This meant that state patients had no access to radiosurgery facilities unless they could afford treatment in the private sector. Consequently, alternative treatment options had to be investigated.
The acquisition of a 6 MV Varian UniqueTM linac equipped with advanced mega voltage-based image-guided radiotherapy (IGRT) software allowed for the implementation of hypofractionated IGRT using non-coplanar dynamic conformal arc (DCA) fields. The decision was taken to utilise this technique for the treatment of small to medium ANs. This study aimed to analyse the radiotherapy treatment plans and quality assurance results for this patient group retrospectively in order to compare these with published data for traditional radiosurgery techniques. In this way, the viability of this approach as an alternative treatment option in under-resourced settings could be investigated. The study was approved by the Human Research Ethics Committee of the University of Cape Town (HREF 104/2016).
Methods and materials
Equipment
The Varian UniqueTM is a 6 MV photon-beam linac equipped with a 120 Millennium multileaf collimator (MLC) allowing 5 mm resolution for central leaves. It is equipped with a high-stability Exact-IGRT couch top. Imaging is undertaken using the PortalVision aS1000 amorphous silicon electronic portal imager with pixel size 0.392 mm.10 IGRT is performed through advanced 2D-2D image matching, allowing for automatic repositioning of patients in longitudinal, lateral and vertical directions. Reported positioning accuracy is within 1.5 mm, with improved results demonstrated with repeated imaging.10 Isocentric stability on the linac is reported to be < 0.6 mm on average, with a maximum deviation of < 1.8 mm.10 The Unique allows for DCA and RapidArcTM (RA) radiotherapy.
Patient population and treatment planning
Fifteen AN patients were treated between February 2013 and January 2016 (eight left- and seven right-sided lesions). All of these patients presented with at least moderate hearing loss on the affected side, with nine having no functional hearing. All were immobilised using a Green ClarityTM fivr-point head and shoulder mask fitted to the CIVCOTM carbon fibre S-frame overlay board. CT and MRI images were fused for all of the patients and treatment planning was performed on the Varian EclipseTM treatment planning system (v11.0) with the analytical anisotropic algorithm (AAA) using a 2 mm calculation grid size. A gross target volume (GTV) to planning target volume (PTV) margin of 2 mm was applied for all patients to allow for the higher expected level of positional uncertainty when compared to traditional radiosurgery treatment options. The mean GTV was 1.6 cc (range 0.6 cc to 9.3 cc), resulting in a mean PTV of 4.0 cc (range 2.3 cc to 15.6 cc). Despite the GTV to PTV margin expansion resulting in a mean increase in volume of 2.3 cc (± 1.36), only 1.1 cc (± 1.01) of this involved brain parenchyma. The remaining margin involved primarily bone and air.
All patients were treated with three non-coplanar DCA fields in three fractions to a total of 19.2 Gy (6.4 Gy × 3 Rx), with one exception, where dose reduction was applied because of tumour size and critical structure constraints (Patient 14; 6.0 Gy × 3 Rx). The prescription dose was planned to coincide with the 80% isodose line. Plans were then renormalised to display coverage of the PTV by the 100% isodose line.
Treatment plan evaluation
Because of the high dose per fraction and the critical location of lesions treated with radiosurgery, plans require a high level of conformity and fast dose fall-off. Several dosimetric indices have been proposed for comparing different radiosurgery plans and modalities, and determining compliance with protocols.
As a first step in the analysis, all plans were evaluated against the Radiation Therapy Oncology Group (RTOG) conformity index (CIRTOG), along with the homogeneity index (HIRTOG) and quality of coverage (QRTOG) in order to verify radiosurgery protocol compliance.11
The CIRTOG is given by
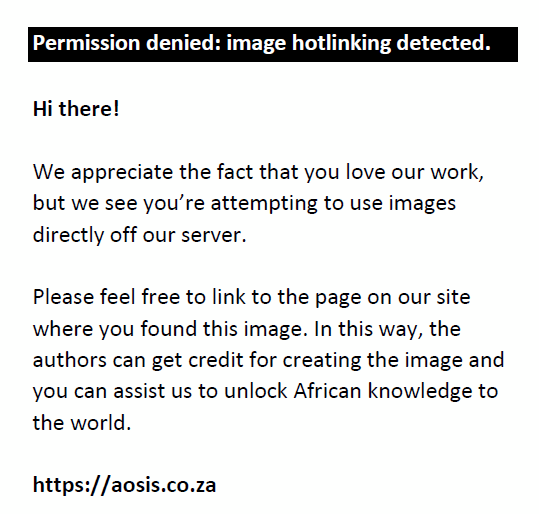
where VRI is the volume encompassed by the prescription isodose, also known as the prescription isodose volume (PIV), and TV is the target volume. The RTOG defines plans with a conformity index between 1.0 and 2.0 as not deviating from protocol, plans with a CIRTOG between 2.0 and 2.5 or between 0.9 and 1.0 as having minor deviations, and plans with a CIRTOG value greater than 2.5 or less than 0.9 as having major deviations from protocol.11,12
The HIRTOG is defined as
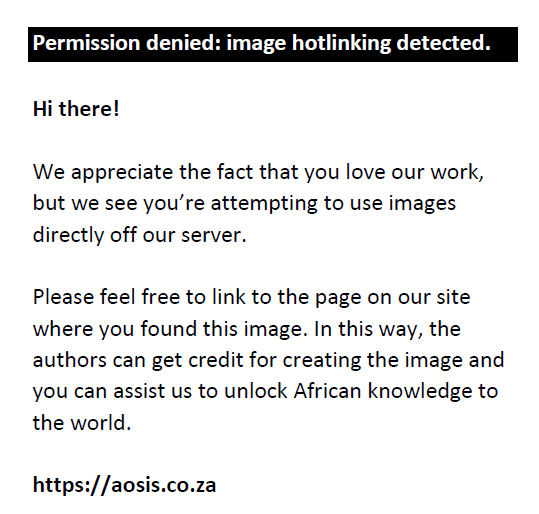
where Imax is the maximum dose in the target and RI is the prescription or reference isodose. Protocol compliance is defined as HIRTOG ≤ 2.0, with a HIRTOG between 2.0 and 2.5 defined as minor and HIRTOG > 2.5 as major deviations.11,12
QRTOG evaluates how well the required dose covers the target and is defined as
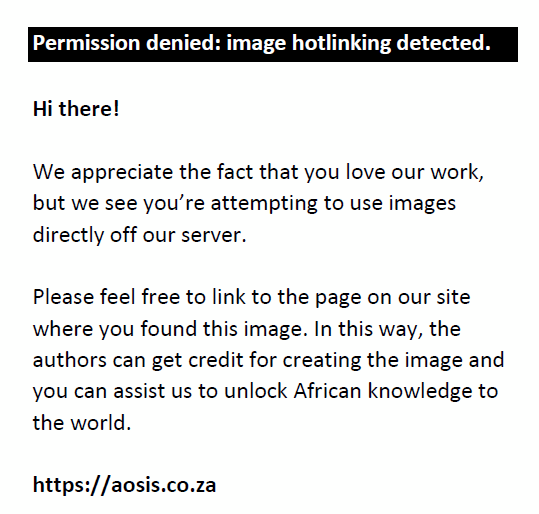
where Imin is the minimum dose received by the target. Protocol compliance requires 90% coverage, with 80% and < 80% coverage defined as minor and major deviations, respectively.11,12
Alternative indices for plan comparison have been proposed because of the risk of ‘false scores’ provided by the more simplistic RTOG indices. As a second step, all plans were analysed using the Paddick conformity and gradient indices (CIPaddick and GIPaddick) and the dose heterogeneity index (DH).13,14,15
The Paddick conformity index (CIPaddick) allows for the simultaneous assessment of conformity and quality of coverage and is defined as
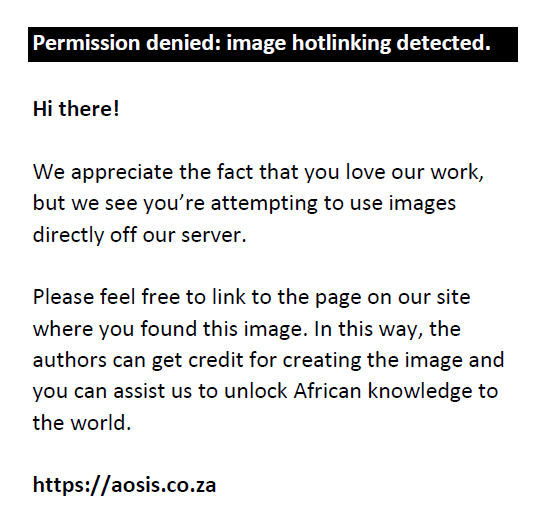
where TV is the target volume, TVPIV is the target volume covered by the PIV, and VRI is the total volume covered by the prescription isodose. It is inversely related to the RTOG conformity index.12,13,15 An ideal plan would result in a CIPaddick of 1.0, with a conformity index of ≥ 0.6 considered acceptable.16
The Paddick gradient index (GIPaddick) attempts to reflect how fast the dose falls off beyond the target in trying to spare normal tissue and critical structures. It is defined as
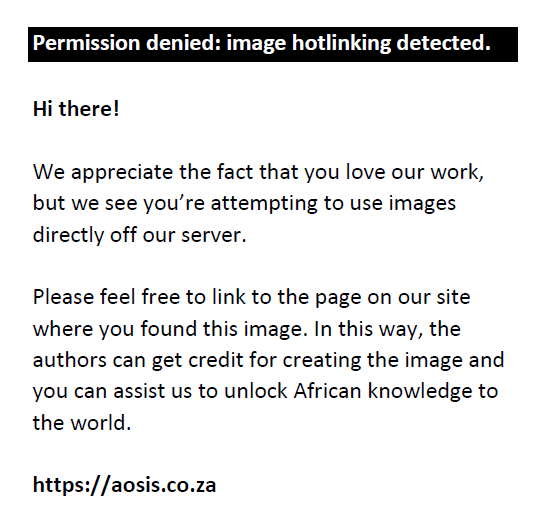
and evaluates the volume of tissue receiving half of the prescription isodose in relation to the volume receiving the prescription isodose.14,15
The dose heterogeneity index (DH) is defined as
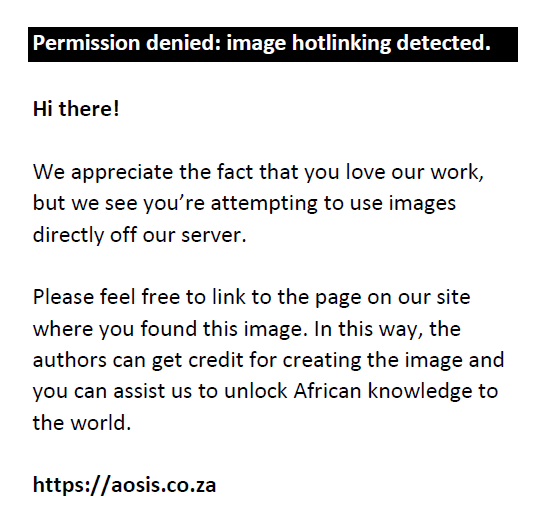
and evaluates dose variation within the tumour volume. An index of zero indicates a homogeneous dose distribution.
Normal tissue and critical structure analysis
Radiosurgery and hypofractionated radiotherapy involve a much higher dose per fraction than conventional radiotherapy. Given the increased risk of late normal tissue complications, extra care must be taken to protect normal brain tissue and organs in close proximity to the tumour. Caution should also be exercised when converting tissue tolerance data based on conventional fractionation and applying it to hypofractionation treatments because of the limitations of the linear quadratic model.17
For ANs, critical structures to consider include normal brain parenchyma, the brainstem, the optic nerve or chiasm, and the cochlea. Maximum doses were recorded for the brainstem, optic pathway and cochlea, and were evaluated based on the normal tissue tolerance guidelines from the AAPM TG101 report.18,19 The risk of radiation-induced necrosis of brain tissue was estimated by evaluating the volume of tissue receiving 12 Gy (V12) or 10 Gy (V10) single fraction equivalent (SFE) dose. The linear quadratic model with α/β = 2 was used to convert 12 Gy SFE and 10 Gy SFE doses to three fraction dose levels (12 GyEq = 19.65 Gy in 3 Rx; 10 GyEq = 16.21 Gy in 3 Rx).19 It is worth noting, however, that because ANs are not central lesions, much of the dose spill falls outside of brain parenchyma. There is no consensus as to whether the V12/V10 volumes should include all tissue, be limited to brain tissue, or whether or not the target volume should be included or excluded.17 Three different V12/V10 dose volumes were therefore assessed in this study: (1) tissue V12/V10 including GTV, (2) brain V12/V10 including GTV, and (3) brain V12/V10 excluding GTV (unaffected brain).
Patient-specific quality assurance and positioning
Film dosimetry was performed on every patient plan prior to treatment delivery to compare predicted and delivered dose. Kodak EDR 2 film was used for coronal plane verification of the composite plan, including the couch, gantry and collimator rotations of the original plan. Film dose calibration was verified through absolute dose measurements performed in a custom designed cylindrical water phantom with a PTW Freiburg GmbH 0.016 cc pinpoint ionisation chamber. PTW VerisoftTM (V5.1) software was used to perform a gamma analysis, adopting dose difference (DD) and distance to agreement (DTA) criteria of 3% and 2 mm.
Individual patient position verification was performed by monitoring the positional shifts required during each setup, and by the final position as recorded on the Varian Portal Vision Advanced Imaging module.
Statistical analysis
All GSH DCA results were analysed to determine deviations from the RTOG radiosurgery criteria. The GSH DCA CIPaddick, GIPaddick and DH results were then compared to the Gamma Knife PerfexionTM, NovalisTM DCA, NovalisTM intensity modulated radiotherapy (IMRT) and CyberKnifeTM results as published by Gevaert et al.15 A one sample t-test compared the GSH mean results for each index to a hypothetical mean – the published values for each index – for each technique.
Results
Radiation Therapy Oncology Group radiosurgery criteria
Analysis of the CIRTOG, HIRTOG and QRTOG values for all patients revealed only one deviation from protocol (Patient 14). This occurred where dose reduction was applied and tumour coverage compromised in order to comply with brainstem dose constraints. The remaining plans were fully compliant with RTOG radiosurgery criteria (Figure 1).
 |
FIGURE 1: Radiation Therapy Oncology Group radiosurgery criteria results for the Groote Schuur Hospital dynamic conformal arc technique. |
|
Study comparison: CIPaddick, GIPaddick, DH
All techniques complied with the minimum published CIPaddick criteria of ≥ 0.6 (Figure 2). The GSH DCA CIPaddick results compared well to those from the Novalis DCA and Novalis IMRT, but were inferior to the Universitair Ziekenhuis Brussel (UZB) published Gamma Knife and CyberKnife results (p < 0.0001).15,16
 |
FIGURE 2: Paddick conformity index comparison between the Groote Schuur Hospital dynamic conformal arc technique and published results from Universitair Ziekenhuis Brussel for CyberKnife, Novalis intensity modulated radiotherapy, Novalis DCA and Perfexion GK techniques. |
|
The largest variation in CIPaddick values was observed for small volumes, with a trend towards better conformity for larger lesions. This finding was not statistically significant.
The results for the GSH DCA gradient index were inferior to all published techniques (Figure 3), with the Novalis IMRT technique being closest, but still superior to the GSH DCA technique (p = 0.0003).
 |
FIGURE 3: Paddick gradient index comparison between the Groote Schuur Hospital dynamic conformal arc technique and published results from Universitair Ziekenhuis Brussel for CyberKnife, Novalis intensity modulated radiotherapy, Novalis DCA and Perfexion GK techniques.15 |
|
With regard to conformity, the gradient index appeared to improve with lesion size. This finding was not statistically significant.
Homogeneity was similar to that reported for the Novalis IMRT and CyberKnife, and proved to be superior to that obtained with the Gamma Knife (p < 0.0001) and Novalis DCA (p = 0.0002).
Normal tissue and critical structure analysis
All critical structures were analysed against the AAPM TG101 criteria, with the tolerances for three fraction treatments listed (Table 1).18,19 Two plans had brainstem volumetric doses exceeding 18 Gy in three fractions (18.31 Gy/3 Rx and 18.71 Gy/3 Rx, respectively; indicated with †), but had maximum point doses within tolerance. Chiasm and optic nerve doses were well below tolerance for all the patients; however, only two had cochlea dose levels below what is described as being required for hearing preservation (doses > 17.1 Gy/3 Rx; indicated with †).
| TABLE 1: Critical structure doses for Groote Schuur Hospital dynamic conformal arc technique. |
The risk of inducing radiation necrosis was assessed using V12Eq and V10Eq data for tissue, brain (including the GTV), and unaffected brain (excluding the GTV). Risk levels from two publications are superimposed in Figure 4.20,21 An increased number of data points were observed above the risk lines for the V10Eq volume analysis compared to the V12Eq analysis. This indicates that the GSH DCA technique may be more sensitive to the V10Eq data, and that analysis of the V12Eq data in isolation may therefore result in under-reporting of the risk of inducing radionecrosis.
 |
FIGURE 4: Volume of tissue, brain (including gross target volume) and unaffected brain (excluding gross target volume) receiving 12 GyEq and 10 GyEq. |
|
Patient-specific quality assurance and patient positioning
Film dosimetry results for the coronal plane showed excellent agreement, with a mean gamma analysis pass rate of 99.8% (± 0.4) with criteria set at 3% DD and 2 mm DTA. The lowest pass rate was 98.7%.
Patient positional shifts were recorded daily. Four treatments required an initial shift of 3 mm and one a 5 mm shift in the longitudinal direction. All other shifts were 2 mm or less, with final mean positional deviation in all three directions < 0.01 cm ± 0.03.
Discussion
Best practice options for radiotherapy as defined in high-income countries are frequently unavailable in LMICs. With population growth expected in many already heavily constrained LMICs, there is both a dire need and an obligation to innovate in order to remove the hurdles to effective care delivery, and to expand available capacity.22 By reviewing patients with small to medium ANs, this study sought to investigate the viability of adopting hypofractionated IGRT using a non-coplanar DCA technique as an alternative treatment approach in under-resourced settings.
The GSH DCA technique was compliant with the RTOG radiosurgery criteria with the exception of a single large-volume treatment, where dose reduction and decreased tumour coverage were accepted in order to obtain critical structure tolerance. The DCA technique also compares favourably with other linac-based techniques for conformity and homogeneity, allowing compliance with minimum standards. This is an important finding given the lack of radiotherapy treatment options in many parts of the world.5,6,7,8
The gradient index results indicate that the dose fall-off is not as steep as that obtained with traditional radiosurgery techniques, as is expected from the larger penumbra obtained with the 5 mm MLC leaves relative to micromultileaf collimators or divergent cones. This results in a greater volume of tissue being included in the V10Eq, thereby potentially increasing the risk of inducing radiation necrosis. It also results in the V10Eq becoming a more sensitive predictor for radiation necrosis than the V12Eq. However, because of the non-central location of the AN lesions, only 7.36 cc (± 4.47) out of the total of 11.01 cc (± 5.34) of V10Eq mean volume actually involved brain parenchyma and target. If the actual GTV is excluded from this V10Eq evaluation, the volume further decreases by a mean of 1.6 cc. The remaining V10Eq dose was deposited in bone, skin and air. This finding may suggest that there is a decreased risk of radiation necrosis for AN patients when compared to radiosurgery patients with other centrally located lesions, where most (or all) of the V12 and V10 volumes are within the brain parenchyma.
Doses to the brainstem and optic system or chiasm were well controlled, but 13 patients did receive a cochlea dose exceeding the recommended maximum tolerance. This may or may not be clinically significant depending on the degree of hearing loss prior to radiosurgery. Clinical follow-up will be required to investigate the potential impact of these doses on the patient group.
The patient-specific quality assurance results indicate a good correlation between the predicted and delivered dose. Variation in final patient position did not exceed 1 mm, thus confirming that the 2 mm GTV to PTV expansion margin was sufficient to allow for the increased inaccuracy in position when compared to traditional radiosurgery techniques.
Conclusion
The GSH DCA technique allows for dosimetrically acceptable treatment of small to medium ANs where hearing preservation is not a clinical factor. In addition, this technique compares favourably with other mainstream radiosurgery techniques when accepted indices are calculated. Care must be taken with critical structures and normal brain parenchyma, with specific reference to the V10Eq volumes. Clinical follow-up is required for the GSH DCA patients to determine long-term treatment outcomes.
Acknowledgements
Competing interests
The authors declare that they have no financial or personal relationships that may have inappropriately influenced them in writing this article.
Authors’ contributions
H.B., principal investigator, is responsible for initial project design, ethics application, data processing and writing of the first draft. H.M.G. is responsible for physics QA for the project, recording and analysis of quality assurance data, and article review. R.B. assisted with project design, methodology, statistical analysis and writing and reviewing of the article. J.D.P., clinical oncologist, is responsible for treatment prescription and planning analysis, critical structure analysis and reporting, writing and reviewing of the article.
References
- Porter RW, Daspit CP, Kresl JJ, Biggs CA, Brachman DG, Syms MJ. Stereotactic radiosurgery in the management of acoustic neuromas. Barrow Q. 2004;20(4):33–39.
- Benghiat H, Heyes G, Nightingale P, et al. Linear accelerator stereotactic radiosurgery for vestibular schwannomas: A UK series. Clin Oncol. 2014;26(6):309–315. https://doi.org/10.1016/j.clon.2014.02.008
- Régis J, Roche PH, Delsanti C, et al. Stereotactic radiosurgery for vestibular schwannoma. In Pollock BE, editor. Contemporary stereotactic radiosurgery: Thechnique and evaluation Armonk. Armonk, NY: Futura Publishing Company, 2002; p. 181–212.
- Rowe J, Radatz M, Walton L, Hampshire A, Seaman S, Kemeny A. Gamma knife stereotactic radiosurgery for unilateral acoustic neuromas. J Neurol Neurosurg Psychiatry. 2003;74(11):1536–1542. https://doi.org/10.1136/jnnp.74.11.1536
- Fezeu F, Awad AJ, Przybylowski CJ, et al. Access to stereotactic radiosurgery: Identification of existing disparities and a modest proposal to reduce them. Cureus. 2014;6(1):e157. https://doi.org/10.7759/cureus.157
- Datta NR, Samiei M, Bodis S. Radiation therapy infrastructure and human resources in low-and middle-income countries: Present status and projections for 2020. Int J Radiat Oncol Biol Phys. 2014;89(3):448–457. https://doi.org/10.1016/j.ijrobp.2014.03.002
- Abdel-Wahab M, Bourque J-M, Pynda Y, et al. Status of radiotherapy resources in Africa: An International Atomic Energy Agency analysis. Lancet Oncol. 2013;14(4):e168–e175. https://doi.org/10.1016/S1470-2045(12)70532-6
- Parkes J. Radiosurgery in South Africa. South African Society of Clinical and Radiation Oncology National Congress. Drakensberg: Champagne Sports Resort; 2013.
- Benatar S. The challenges of health disparities in South Africa. S Afr Med J. 2013;103(3):154–155. https://doi.org/10.7196/SAMJ.6622
- Clivio A, Nicolini G, Vanetti E, Fogliata A, Cozzi L. Commissioning and early experience with a new-generation low-energy linear accelerator with advanced delivery and imaging functionalities. Radiat Oncol. 2011;6(1):1. https://doi.org/10.1186/1748-717X-6-129
- Shaw E, Kline R, Gillin M, et al. Radiation Therapy Oncology Group: Radiosurgery quality assurance guidelines. Int J Radiat Oncol Biol Phys. 1993;27(5):1231–1239. https://doi.org/10.1016/0360-3016(93)90548-A
- Stanley J, Breitman K, Dunscombe P, Spencer DP, Lau H. Evaluation of stereotactic radiosurgery conformity indices for 170 target volumes in patients with brain metastases. J Appl Clin Med Phys. 2011;12(2):245–253. https://doi.org/10.1120/jacmp.v12i2.3449
- Paddick I. A simple scoring ratio to index the conformity of radiosurgical treatment plans: Technical note. J Neurosurg. 2000;93(Suppl 3):219–222.
- Paddick I, Lippitz B. A simple dose gradient measurement tool to complement the conformity index. J Neurosurg. 2006;105(7):194–201.
- Gevaert T, Levivier M, Lacornerie T, et al. Dosimetric comparison of different treatment modalities for stereotactic radiosurgery of arteriovenous malformations and acoustic neuromas. Radiother Oncol. 2013;106(2):192–197. https://doi.org/10.1016/j.radonc.2012.07.002
- Lawrence M, Rossi P, Powell D, et al. Relationship between Radiosurgery Conformity Indices and Acoustic Neuroma Tumor Volume. In McDermott MW, editor. Radiosurgery. Volume 7. Karger, 2010; p. 95–99. https://doi.org/10.1159/000288722
- Milano MT, Usuki KY, Walter KA, Clark D, Schell MC. Stereotactic radiosurgery and hypofractionated stereotactic radiotherapy: Normal tissue dose constraints of the central nervous system. Cancer Treat Rev. 2011;37(7):567–578. https://doi.org/10.1016/j.ctrv.2011.04.004
- Benedict SH, Yenice KM, Followill D, et al. Stereotactic body radiation therapy: The report of AAPM Task Group 101. Med Phys. 2010;37(8):4078–4101. https://doi.org/10.1118/1.3438081
- Khan FM, Gerbi BJ, editors. Treatment planning in radiation oncology 2012. Philadelphia, PA: Wolters Kluwer/Lippincott Williams & Wilkins Health.
- Minniti G, Clarke E, Lanzetta G, et al. Stereotactic radiosurgery for brain metastases: Analysis of outcome and risk of brain radionecrosis. Radiat Oncol. 2011;6(1):1. https://doi.org/10.1186/1748-717X-6-48
- Blonigen BJ, Steinmetz RD, Levin L, Lamba MA, Warnick RE, Breneman JC. Irradiated volume as a predictor of brain radionecrosis after linear accelerator stereotactic radiosurgery. Int J Radiat Oncol Biol Phys. 2010;77(4):996–1001. https://doi.org/10.1016/j.ijrobp.2009.06.006
- Atun R, Jaffray DA, Barton MB, et al. Expanding global access to radiotherapy. Lancet Oncol. 2015;16(10):1153–1186. https://doi.org/10.1016/S1470-2045(15)00222-3
|